Development of a Home-Based Pharmaceutical Care Model for End-of-Life Palliative Patients in the Primary Care Network of Hatyai Hospital
Keywords:
model development, pharmaceutical care, terminally ill patients, home-based continuityAbstract
Background: End-of-life patients receiving home-based palliative care require continuous medication management and ongoing symptom monitoring. However, the current healthcare system lacks an established model for continuous pharmaceutical care at home within the context of the primary care service network.
Objective: To develop a model of continuous home-based pharmaceutical care and to evaluate its outcomes.
Methods: This study employed an action research design conducted between February 1, 2025, and September 30, 2025. The research comprised two phases: (1) development of the care model through focus group discussions based on the six health system building blocks framework, and (2) evaluation of the model’s implementation among end-of-life patients receiving home-based palliative care. Data were analyzed using descriptive statistics. Comparisons of symptom burden before and after pharmacist involvement were performed using paired t-tests or Wilcoxon signed-rank tests, depending on data distribution. Caregiver satisfaction before and after the intervention was analyzed using paired t-tests.
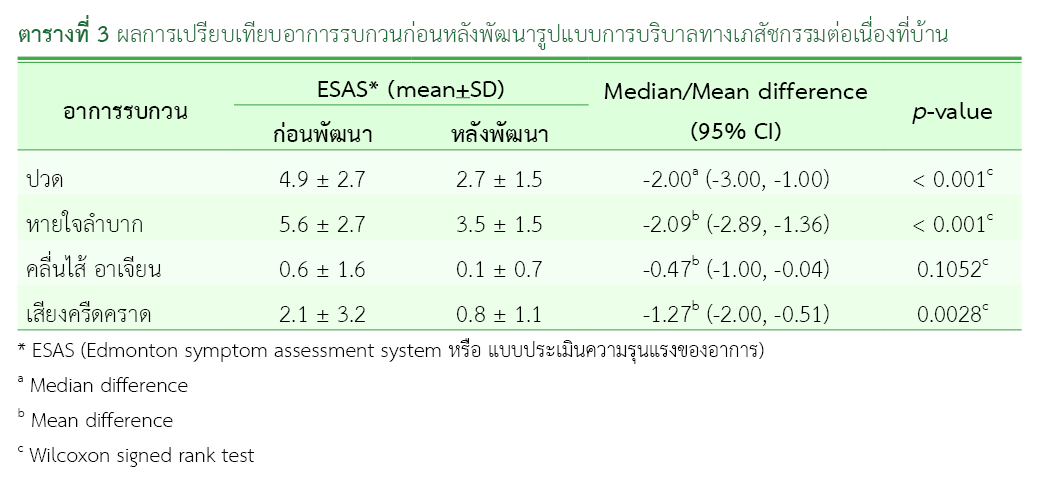
Results: The developed pharmaceutical care model enhanced continuity of care outside regular working hours and improved access to 24-hour symptom management. Pain, dyspnea, and terminal respiratory secretions were significantly reduced following implementation (p-value < 0.05). Modifications to strong opioids regimens and routes of administration were made to better align with patients’ clinical conditions. Caregiver satisfaction scores increased significantly from 3.38 ± 0.55 to 4.81 ± 0.28 (p-value < 0.001). In contrast, satisfaction among healthcare providers increased from 4.14 ± 0.34 to 4.41 ± 0.57; however, this difference was not statistically significant (p-value > 0.05).
Conclusion: Integrating primary care pharmacists into home-based palliative care through telemedicine shows promise in improving symptom management outcomes, medication safety, and continuity of care for end-of-life patients.
References
Dokmai P, Meemon N, Paek SC, Tayjasanant S. Structure and process of palliative care provision: a nationwide study of public hospitals in Thailand. BMC Health Serv Res. 2021;21(1):616. doi: 10.1186/s12913-021-06623-w.
Nilmanat K. Palliative care in Thailand: Development and challenges. Can Oncol Nurs J. 2016;26(3):262–4. PMID: 31148701.
Geiger J, Enck G, Luciani L, Fudin J, McPherson ML. Evolving roles of palliative care pharmacists. J Pain Symptom Manage. 2022;64(6):e357–61. doi: 10.1016/j.jpainsymman.2022.07.012.
Moody JJ, Poon IO, Braun UK. The role of an inpatient hospice and palliative clinical pharmacist in the interdisciplinary team. Am J Hosp Palliat Care 2022;39(7):856–64. doi: 10.1177/10499091211049401.
Sabrouty RE, Elouadi A, Salifou Karimoune MA. Remote palliative care: a systematic review of effectiveness, accessibility, and patient satisfaction. Int J Adv Comput Sci Appl. 2024;15(5):502–13. doi: 10.14569/IJACSA.2024.0150550.
Cipolle RJ, Strand LM, Morley PC. Pharmaceutical care practice: the patient centered approach to medication management service. 3rd ed. New York: McGraw-Hill; 2012.
Chewaskulyong B, Sapinun L, Downing GM, Intaratat P, Lesperance M, Leautrakul S, et al. Reliability and validity of the Thai translation (Thai PPS adult Suandok) of the palliative performance scale (PPSv2). Palliat Med. 2012;26(8):1034-41. doi: 10.1177/0269216311424633.
Chinda M, Jaturapatporn D, Kirshen AJ, Udomsubpayakul U. Reliability and validity of a Thai version of the Edmonton symptom assessment scale (ESAS-Thai). J Pain-Symptom Manage. 2011;42(6):954-60. doi: 10.1016/j.jpainsymman.2011.02.020.
World Health Organization. Monitoring the building blocks of health systems: a handbook of indicators and their measurement strategies [Internet]. Geneva: World Health Organization; 2010 [cited 2025 Jan 22]. Available from: https://cdn.who.int/media/docs/default-source/service-availability-and-readinessassessment%28sara%29/related-links-%28sara%29/who_mbhss_2010_cover_toc_web.pdf
Krumm L, Bausewein C, Constanze Rémi. Drug therapy safety in palliative care - pharmaceutical analysis of medication processes in palliative care. Pharmacy (Basel). 2023;11(5):160. doi: 10.3390/pharmacy11050160.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Health Administration Division, Office of the Permanent Secretary, Ministry of Public Health and The Society of Hospital Pharmacist, Ministry of Public Health

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
ข้อความภายในบทความที่ตีพิมพ์ในวารสารเภสัชกรรมคลินิกทั้งหมด รวมถึงรูปภาพประกอบ ตาราง เป็นลิขสิทธิ์ของกองบริหารการสาธารณสุข สำนักงานปลัดกระทรวงสาธารณสุข และ ชมรมเภสัชกรโรงพยาบาลกระทรวงสาธารณสุข การนำเนื้อหา ข้อความหรือข้อคิดเห็น รูปภาพ ตาราง ของบทความไปจัดพิมพ์เผยแพร่ในรูปแบบต่าง ๆ เพื่อใช้ประโยชน์ในเชิงพาณิชย์ ต้องได้รับอนุญาตจากกองบรรณาธิการวารสารเภสัชกรรมคลินิกอย่างเป็นลายลักษณ์อักษร
กองบริหารการสาธารณสุข สำนักงานปลัดกระทรวงสาธารณสุข และ ชมรมเภสัชกรโรงพยาบาลกระทรวงสาธารณสุข อนุญาตให้สามารถนำไฟล์บทความไปใช้ประโยชน์และเผยแพร่ต่อได้ โดยอยู่ภายใต้เงื่อนไขสัญญาอนุญาตครีเอทีฟคอมมอน (Creative Commons License: CC) โดย ต้องแสดงที่มาจากวารสาร – ไม่ใช้เพื่อการค้า – ห้ามแก้ไขดัดแปลง, Attribution-NonCommercial-NoDerivatives 4.0 International (CC BY-NC-ND 4.0)
ข้อความที่ปรากฏในบทความในวารสารเป็นความคิดเห็นส่วนตัวของผู้เขียนแต่ละท่านไม่เกี่ยวข้องกับกองบริหารการสาธารณสุข สำนักงานปลัดกระทรวงสาธารณสุข และ ชมรมเภสัชกรโรงพยาบาลกระทรวงสาธารณสุข และบุคลากรในกองฯ หรือ ชมรมฯ แต่อย่างใด ความรับผิดชอบองค์ประกอบทั้งหมดของบทความแต่ละเรื่องเป็นของผู้เขียนแต่ละท่าน หากมีความผิดพลาดใด ๆ ผู้เขียนแต่ละท่านจะรับผิดชอบบทความของตนเอง ตลอดจนความรับผิดชอบด้านเนื้อหาและการตรวจร่างบทความเป็นของผู้เขียน ไม่เกี่ยวข้องกับกองบรรณาธิการ



